What is a joint injection?
The foot and ankle is a complex structure composed of many joints and soft tissues. Injections can help pinpoint which is causing your symptoms. This can help to confirm and treat your diagnosis. The procedure introduces steroid and local anaesthetic into a joint. This is useful in conditions such as arthritis and when scar tissue is present within the joint. The goals of a joint injection are to relieve pain and improve joint function.
How does the joint injection work?
The local anaesthetic typically provides pain relief within the first day. The steroid reduces inflammation and will take longer to work. When joints are painful, often due to arthritis, the joint lining is inflammed with an increased blood supply. The steroid aims to break the cycle of inflammation so that the pain nerves are no longer stimulated. This takes 6-8 weeks to take effect. If the inflammation is reduced it is possible that the pain can resolve for a long time. However, the joint can become inflammed again sometime after the injection, and the pain may come back. In this case it is useful to know if the injection helped even for a short time as this confirms that the joint injected is the one causing the pain, and suggests surgery may help further.
The steroid only works within the joint and has no systemic effects, that are commonly associated with steroid tablets.
How is the injection done?
Most people have the injection performed under local anaesthetic whilst they are awake. Depending on the location, Mr Davda may be able to do this in the clinic, or it may have to be done in the radiology department with the help of an ultrasound or xray machine. Using these machines helps to pinpoint the exact area causing pain and ensure the needle is in the right place. The skin over the joint will be cleaned and sterilised with commonly used agents like topical iodine. The medication will be injected using a syringe and needle. The injection site may need to be covered with a bandage or have pressure applied for a few minutes.
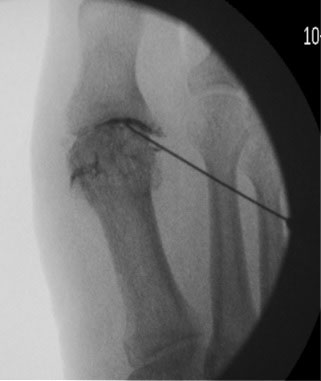
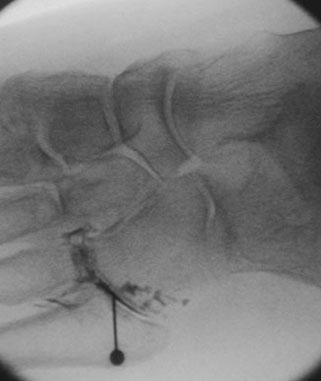
The images above are xrays taken at the time of a injection. The first image shows the dye used to locate the big toe joint. Whilst the dye is clear to the naked eye, it appears black when an xray is taken. The second image shows an injection into the outer midfoot.
Some joints in the foot are so small that it may not be possible to safely deliver the injection with the patient awake. In this case, the injection will be performed on a scheduled day in the operating theatre. The patient may require sedation or a general anaesthetic.
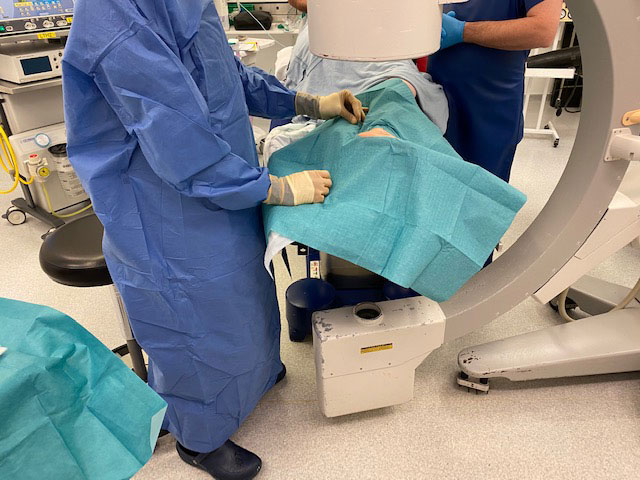
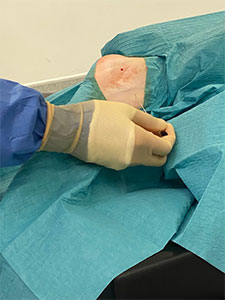
The photos above are taken with a patient asleep in theatre. In the case. Mr Davda is performing an injection into the joint between the ankle and heel with the use of an xray machine.
When should I avoid a joint injection?
Joint injection should be avoided in certain situations. Some of these include the presence of skin or blood infections and a history of allergic response to injectable medications.
In addition, Mr Davda may rule out a joint injection if there was little improvement after a previous injection; if you have a bleeding disorder or are on blood thinning medication; you have poorly controlled diabetes, or your body has problems fighting infections.
What happens after a joint injection?
You may be asked to stay in the hospital for a short while to be observed for side effects of the injection. You may be instructed to avoid or limit activity for a day or so after the injection. It is helpful to keep a diary of your symptoms for us to understand how well the injection worked.
Some commonly asked questions
What are the potential complications of a joint injection?
Your symptoms may worsen for a short period in the days after the injection, but usually settle within a few weeks. This occurs in about 2 of every 100 patients.
Complications include infection of the skin at the injection site, infection of the joint, tenderness, swelling and warmth. There can sometimes be nerve or blood vessel injury, or damage to the joint surfaces.
Steroids may cause loss skin discolouration or thinning of the skin, weakening of a nearby ligament or tendon with the possibility of complete tears.
The steroid injection only affects the joint involved and will not have long last lasting systemic effect. The injection can temporarily increase blood sugar levels in diabetics and disrupt the body’s own steroid hormone balance, particularly in patients with hormone disorders.
Local anaesthetic may cause flushing, hives, chest or abdominal discomfort, and nausea. Contrast agent may cause allergic reaction.
The complications described above are uncommon, and typically occur in less than 1 in 100 cases.
How long will the injection last for?
The period of pain relief will vary according to the condition that is being treated. Most injections will last for a minimum of 3 months and in some cases for several years.
Hoe many injections can I have?
There is no single consensus on how often one should have injections. As a general guide, I would recommend no more than two injections over a 12 month period.
Will I be able to drive after the injection?
Yes you will be able to drive. There are no restrictions on driving.
How should I clean the injection site at home?
No specific cleaning of the injection site is typically needed. You are able to resume normal showering or bathing after joint injections.
Will it interfere with my other medications?
You doctor will be able to answer this question for you. Be sure to bring a current list of your medications to your appointment.
Will a steroid injection raise my blood sugar?
If you are diabetic, a joint injection with steroid may cause your blood sugar to be increased for a short time
