What is Morton’s Neuroma?
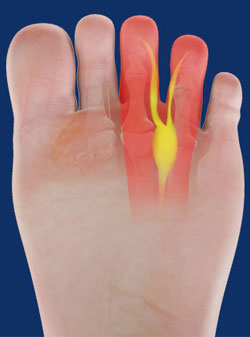
This is a painful benign swelling or irritation of the digital nerve that runs between the metatarsal bones of the foot. Entrapment of this nerve causes pain in the ball of the foot that radiates to the toes and is sometimes described as feeling like walking on a pebble or marble. The condition is named after Dr Thomas Morton who described it in 1876.
How is the neuroma caused?
In many cases, a neuroma may develop from excessive loading on the front of the foot. This can occur in those who regularly wear high heels with a narrow toe box. Patients will often feel more comfortable out of shoes. The underlying shape and alignment of the foot, as well as tightness in the calf muscle, may contribute to the overload. There may be some cases where the neuroma develops spontaneously with no obvious reason.
What are the symptoms?
Pain, numbness and a tingling sensation in the toes are the main symptoms. This usually presents when the foot is enclosed in a shoe and while standing or walking. The condition commonly affects the 3rd and 4th toes and sometimes the 2nd and 3rd toes. As the condition progresses, shooting pains (like electric shocks) may be felt, even while not weight bearing. Occasionally a ‘clicking’ sensation is associated with the pain. Other conditions such as inflammation within the toe and foot joints (known as synovitis), or inflammation within the soft tissue (known as bursitis) can present with similar symptoms.
Assessment
The diagnosis may be difficult and much depends on the history and description of the problem. Patients with classic Morton’s neuroma will have pain with pressure at the base of the involved toes. In addition, squeezing the front of the foot together, known as Mulder’s Test, can exacerbate symptoms. There may be numbness on the sides of one toe and the adjacent toe, as this corresponds with the distribution of the involved nerve. Tightness of the calf muscle will also be tested for as this may contribute to the cause of the neuroma. Conditions such as nerve entrapment around the ankle and diabetes may present with similar numbness around the forefoot and will be examined for.
Imaging
Weight bearing radiographs (x rays) may be taken to examine the shape of the foot, length of the underlying foot bones and look for arthritis in the foot joints. Mr Davda may request an ultrasound scan to be done. This will be performed by a musculoskeletal radiologist in the radiology department on a separate occasion to your clinic appointment. The scan involves using sound to generate an image of the soft tissue between the metatarsals. Local anaesthetic and steroids may be administered by the radiologist during the scan and the doctor will ask you to keep a pain diary to see if your symptoms are relieved.
Unusually, if diagnosis proves difficult, an MRI (magnetic resonance imaging scan) may be carried out to examine for other causes of your symptoms.
Treatment
Conservative
The vast majority of Morton’s neuroma can be treated with conservative measures with no operation required. These include:
Appropriate shoes and orthotics
This is directed at modifying footwear and insoles. Extra wide soft shoes with cushioning to the soles often help to offload the forefoot.
Stretching exercises
Sustained stretching exercises of a tight calf muscle over the period of several months, will help to off load the forefoot when walking.
Steroid injection in conjunction with a local anaesthetic (lignocaine) injected into the area around the nerve relieves pain in a high number of cases. As mentioned above, this is usually performed with ultrasound guidance and is now rarely performed blind in the clinic setting. The injection may take several weeks to work, and in a small number of cases may exacerbate symptoms before making them better.
Surgery
If the non operative treatments described above are unsuccessful surgery may be necessary. This has about an 80% success rate.
Before surgery
Your fitness for surgery and your foot and ankle symptoms will be reassessed in our pre assessment clinic, which usually takes place prior to the date of operation. Blood tests and further investigations of the heart and lungs may be required to ensure you are fit to have a general anaesthetic. If you live alone, we will liaise with your GP and social services to ensure that care is in place to look after you following surgery. Occasionally, you may need to spend a few extra days in hospital whilst the services are being organised.
We kindly ask that you contact us if you suffer an insect bite, cut or bruise to the symptomatic foot in the period leading up to your surgery, or if you have been unwell. Any injury to the skin in the area of your intended surgery can increase the risk of infection. You may need reassessment and surgery reorganised for another time.
On the day of the surgery
You will be seen before surgery by Mr Davda or team member to check your consent and mark the leg. Neuroma surgery is typically performed under general anaesthetic, which can be discussed with your anaesthetist.
You will be able to go home the same day. Sometimes, it is necessary to spend a night in hospital depending on your general health and immediate recovery from the operation. Local anaesthetic is also applied at the time of surgery to provide pain relief and numb the foot. This can last for up to a day after.
The operation
The operation involves removing part of the nerve that causes pain and discomfort. The surgery is performed under general anaesthetic, through a small incision on the top of the foot, between the affected toes. The neuroma is typically the size of a pea and found between the metatarsal bones. As part of the nerve is removed some permanent numbness will be experienced on the side of the involved toes. In about 5% of patients persistent pain occurs at the cut end of the nerve and further surgery is required. This is known as a stump neuroma. In view of this, surgery is only considered after all non-operative measures have been tried. In the rare circumstance that there are two adjacent neuromas, the most symptomatic one will be removed and the ligament overlying the second will be released.
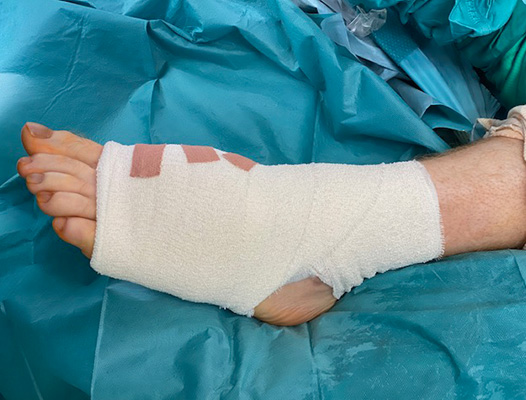
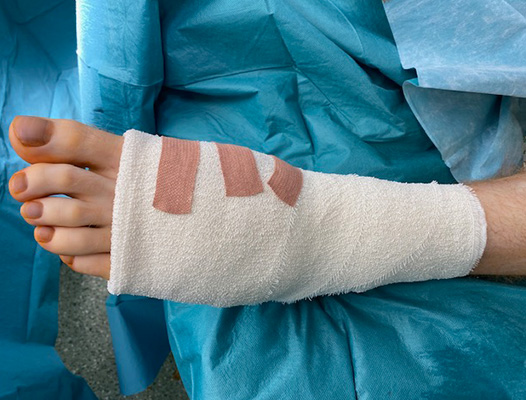
The photos above show the typical post operative bandaging applied to the foot following surgery.
After the operation
It is not uncommon for the wound to bleed a little and stain the bandaging, particularly when standing for the first time after the operation. For the first two weeks following surgery you are advised to elevate the foot on 2-3 pillows to help reduce any swelling and promote healing of the wound. It is best to keep walking and weight bearing to a minimum and only for essential purposes. You should avoid getting the foot and bandages wet whilst bathing. The foot can be covered with a plastic bag or a special covering available online. You will be seen by Mr Davda in the clinic 2 weeks after the operation, where the bandaging will be removed and the wound checked.
Common Questions
When can I drive?
Patients having had their left foot operated on will usually be able to drive an automatic car within a week. Those who have had an operation on the right side will be able to drive after the banding has been removed in the post operative appointment. You are advised to contact your insurance company to ensure you are covered to drive.
When can I go back to work?
This will depend on the type of work you do. For example, if you have a desk job you may be able to return to work in 1-2 weeks provided you are able to rest and elevate your foot whilst sitting. If you do a physically demanding job, you will need 3 – 4 weeks off.
When can I return to sport?
You can usually return to sport 6 weeks from the date of surgery. Recreational walking or light sporting activity can be resumed earlier.
Complications
Swelling
This is very common after surgery. It is a side effect, rather than a complication, and can take up to a year to recover. You may need a shoe size slightly larger than you normally wear during this period.
Infection
This can occur in a small percentage of patients. Minor infections normally settle after a short course of antibiotics.
Numbness and tingling
This occurs at the surgical site, as a result of minor nerve damage and usually recovers over the course of six months. Persistent pain may be related to a stump neuroma as described above and will need to be investigated for if symptoms persist.
Blood clots
A clot in the calf of the operated foot (known as deep vein thrombosis or DVT), or a clot in the lung (known as pulmonary embolus or PE) is rare. Please inform the team if you have had a DVT or PE before, or if you have a family history of clotting disorders. You may require a short course of a blood thinning injection if this is the case, or if we are operating on both feet at the same time.
Complex regional pain syndrome
On rare occasions, surgery to the foot can upset the overall nerve supply and cause a sensation of burning and tingling, with change in colour of the foot. This typically presents 2-3 months after surgery and can be troublesome. Fortunately, this complication is extremely uncommon, occurring very rarely.
