What is a Lisfranc Injury?
The Lisfranc joint is found at the base of the first and second metatarsal bones, in the middle of the foot. A strong ligament, known as the Lisfranc ligament, spans across the joint. This provides substantial stability to the midfoot.
The injury is named after the 19th century French surgeon Jaques LisFranc de St. Martin, who described this when soldiers were knocked off of their horses with their feet caught in the stirrup.
Causes
A Lisfranc injury can occur due to the twisting of the foot (low-energy injury), a fall from a height or a traumatic motor accident (high-energy injury).
Symptoms
Lisfranc injuries are characterised by pain and the inability to bear weight. The appearance of bruises and swelling across the midfoot may occur. The injury is often mistaken for a foot sprain and is often missed on initial presentation.
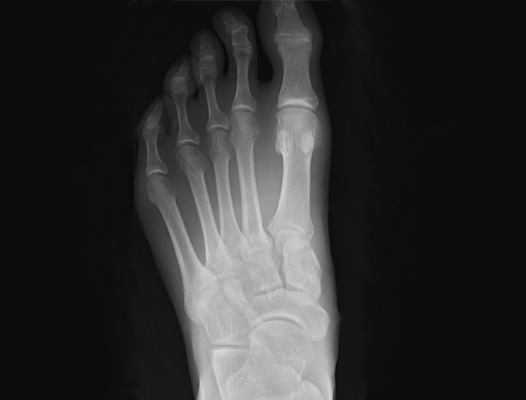
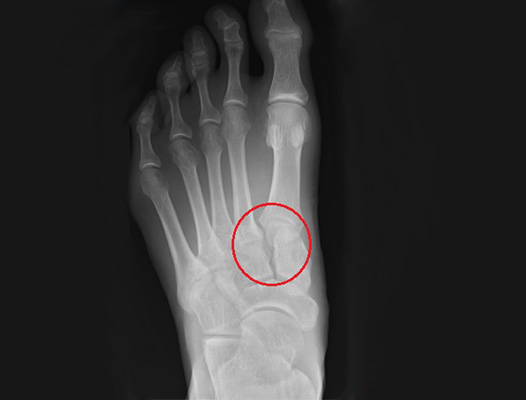
Diagnosis
Mr Davda will first take a thorough history and examine the physical condition of the foot by inspection and palpation (feeling) and then order X-rays. These X-rays will be taken with the patient standing and bearing weight through the foot if possible. This allows assessment of the stability of the Lisfranc joint when bodyweight is placed through it. Further imaging with a CT or MRI scan maybe required to provide more information about the injury and state of the adjacent joints.
Treatment
Conservative
Imaging and symptoms will help to identify if the Lisfranc injury can be treated conservatively, or with surgery. The early stages of injury can be treated with rest, application of ice, elevation of the foot and simple analgesia. The foot and leg may need to be kept in a cast or boot inorder to allow the injury to settle and heal. This is the case in stable and ‘undisplaced’ injuries where the overall alignment of the foot has not been disrupted.
Surgical
If the xrays and scans show the injury has caused a widening of the midfoot joints or change in alignment, surgery will be required. This is often evident acutely when the injury has occurred, but can also begin to appear in subtle cases many months from the time of injury.
Before surgery
Your fitness for surgery and your symptoms will be reassessed in our pre assessment clinic, which takes place prior to the date of operation. Blood tests, as well as further investigations of the heart and lungs may be required to ensure you are fit to have a general anaesthetic. If you live alone, we will liaise with your GP and social services to ensure that care is in place to look after you following surgery. Occasionally, you may need to spend a few extra days in hospital whilst the services are being organised.
We kindly ask that you contact us if you suffer an insect bite, cut or bruise to the symptomatic leg in the period leading up to your surgery. Any injury to the skin in the area of your intended surgery can increase the risk of infection. You may need reassessment and surgery reorganised for another time.
On the day of surgery
You will be seen by Mr Davda or a member of the team to check your consent and mark the leg. Lisfranc surgery usually takes several hours to and is commonly performed under general anaesthetic. Local anaesthetic is also applied at the time of surgery to provide pain relief and numb the foot. This can last for up to a day after. The anaesthetist will discuss this further with you on the day of surgery.
You will be in hospital overnight, and will not be discharged until your post operative pain is under control and the physiotherapists are satisfied with your mobility.
The Operation
The surgery is typically performed through an incision on top of the midfoot. Further incisions maybe required if additional injuries need fixing. The Lisfranc joint is secured with a combination of plates and screws that correctly align the bones of the midfoot. An example is shown below. An xray machine is used at the time of surgery to ensure the screws are in the correct position. A cast is applied at the end of the operation and will normally stay on for 6 weeks. It will be changed 2 weeks following surgery inorder to check the wounds.
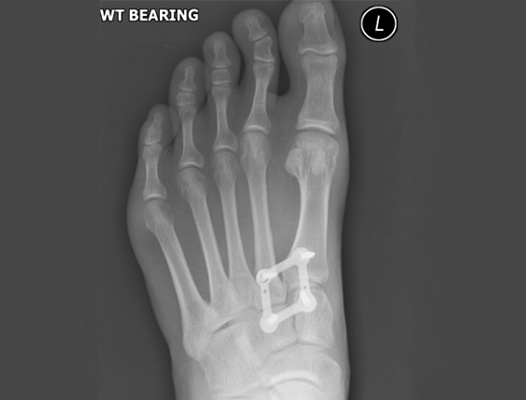
After The Operation
The foot and ankle will feel numb from the local anaesthetic for the first few hours following surgery. I encourage you to take painkillers as soon as possible, as the numbness will gradually fade over time.
You will need to have a blood thinning injection every evening for the duration of time in the cast, typically 6 weeks. You or your carer will be shown how to do this on the ward by the nursing staff. Before you leave hospital, our physiotherapists will show you how to walk with crutches or a frame.
For the first two weeks following surgery you are advised to elevate the leg on 2-3 pillows, above the level of the chest. This will help reduce swelling and promote healing of the wounds.
Will I able to walk after the operation?
Your leg will be in a cast for the first six weeks following surgery and you will remain NON WEIGHT BEARING. At this stage, an xray will be taken to ensure the injury has healed. Once the cast is taken off, you may be placed into a walking boot and physiotherapy will begin.

You may require a longer period in cast if the foot is slow to heal, or you have an underlying condition such as diabetes, or you are a smoker.
When can I drive?
Patients having had the left foot operated on will be able to drive an automatic car within 2-3 weeks (short distances only to avoid swelling). Those who have had an operation on the right side will be able to drive after about 8-10 weeks. You are advised to contact your insurance company to ensure you are covered to drive.
You are advised not to fly after surgery for six weeks (short haul) and 12 weeks (long haul).
When can I go back to work?
This will depend on the type of work you do. For example, if you have a desk job you may be able to return to work after two weeks provided you are able to rest and elevate your foot whilst sitting. If you do a physically demanding job, you will need a minimum of 12 weeks off.
Possible Complications of Surgery
Swelling
This is very common after surgery. It is a side effect, rather than a complication, and can take up to a year to recover. You may need a shoe size slightly larger than you normally wear during this period.
Wound healing
The skin along the top of the foot is relatively thin and delicate. Unlike an arm or thigh, there is little protective muscle or soft tissue underneath, hence it is more prone to infection or wound healing issues.
Infection
This can occur in a small percentage of patients. If this is the case, it is possible that further surgery may be required to remove infected bone or screws. Minor infections are commoner and normally settle after a short course of antibiotics.
Numbness and tingling
This can occur at the surgical site as a result of minor nerve damage and usually recovers over the course of six months.
Metalwork impingement
Prominent screws that can be felt through the skin or cause irritation may be removed at a later stage, typically a year after the initial procedure. Metalwork is not removed unless it is symptomatic.
Blood clots
A clot in the calf of the operated foot (known as deep vein thrombosis or DVT), or a clot in the lung (known as pulmonary embolus or PE) is rare. Please inform the team if you have had a DVT or PE before, or if you have a family history of clotting disorders. You will be on blood thinning medication for the time you are in cast.
Arthritis
If the surgical treatment fails or the joint damage from the injury leads to severe arthritis, then a fusion (arthrodesis) of the Lisfranc joint may be necessary. Despite the stiffness of a fused joint, most patients with successful fusion of the midfoot joints have good function of the foot.
