What is a stress fracture?
A stress fracture is a small hairline crack or break typically seen in weight bearing bones, such as in the leg bone (called the tibia) or in the foot. It is typically related to overuse and an new level of weight bearing activity
What are the symptoms?
A dull aching type pain is usually felt over the affected area and tends to develop gradually. It is made worse by placing weight through the affected side and made better by resting. The pain may worsen with time and occur during the day and night. The affect area may be swollen, tender to touch and you may have difficulty any weight through it.
How does a stress fracture develop?
Like skin and muscle, bone is a living tissue. It continually replaces older bone with new and healthy bone in a process known as ‘remodelling’. Thus, bone adapts to the load that is placed through it, but takes time to do so.
When bone is exposed to new levels of loading which is beyond it’s normal capacity, microscopic cracks can begin to appear as the bone is stressed. An example of increased levels of activity would be when taking up running for a marathon, or long daily walks. Your bone has not had sufficient time to remodel and form newer stronger bone. These cracks can eventually form a fracture if activity levels are not reduced. Stress fractures may also occur where the bone is weakened or abnormal, such as in the presence of low vitamin D, abnormal thyroid hormone levels or osteoporosis. Smoking and diabetes are also known associations.
Stress fractures tend to occur in certain weight bearing bones, and particular locations within those This is because some bones have distinct areas called ‘watershed zones’ that are less richly supplied with blood as others. Hence, these areas have less potential for healing. Each person will absorb forces placed through their feet in a slightly different manner and this is dictated by the foot shape, alignment and gait pattern. Common sites of stress fractures in the foot include:
- Metatarsal Neck Region
- Base of the 5th metatarsal
- Sesamoid bones of the Great Toe
- Navicular
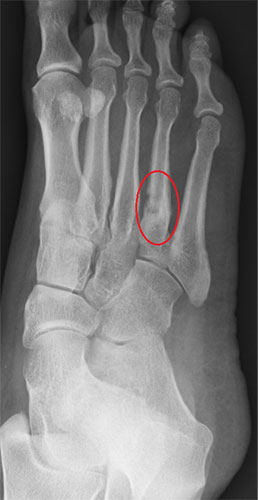
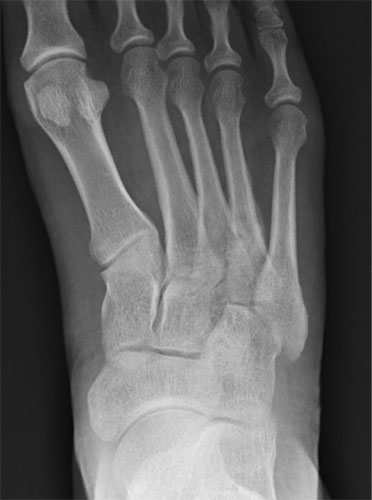
The xray above show a stress fracture of the fourth metatarsal highlighted by the red circle.
Diagnosis
A clear and thorough history will be taken by Mr Davda. Initial X-rays may not demonstrate any abnormalities in the first few weeks of the symptoms as it often takes 10 days or more for a callus (new bone) to form and be visualized on x-rays. Bone scans and MRIs are more likely to be positive in stress fractures. It is common to see fluid or “oedema” in bones on an MRI without having an obvious stress fracture. This represents a “stress reaction” and is equivalent to microscopic bone fracturing without a complete stress fracture. The fracture, if present, is usually visible on an MRI. If there is a concern, a CT scan can usually confirm the diagnosis of stress fracture, as well as clearly define the location and size of the fracture.
Treatment
Most stress fractures do not require surgery. Treatment generally involves:
- Metabolic and systemic factors
Blood tests will be taken to measure Vitamin D levels, calcium and other possible causes of stress fractures such as thyroid levels.
Low Vitamin D is extremely common and an easily treated condition. The recommended daily dosage is 1000 units daily, however a loading regime of 3-5000 units can be safely given for a period of time. Vitamin D is available over the counter in your local pharmacy, often combined with calcium.
- Off loading and resting the leg
Resting the affected area until the bone adequately heals, often takes 6-8 weeks or more. This can be accomplished with non weight bearing, using crutches or a walking boot. Mr Davda will recommend the most appropriate treatment for the timeline. Avoid activities that may have caused the stress fracture.
- Maintaining fitness
This is best achieved through avoiding load bearing activities such as long distance walking or running. Cross training, swimming and cycling are better exercises as this lessens the impact on the bone.
- Biomechanical factors
Mr Davda will examine your limb alignment, foot shape and tightness of the calf muscle which can predispose to overloading of the forefoot. Physiotherapy and stretching exercises to alleviate calf tightness can be found here.
Surgery
Surgery is rarely indicated in stress fractures. Certain “high risk” stress fractures include the Jones fracture, or a displaced navicular stress fracture, which may not heal adequately without surgery. This will be discussed in greater detail with you.
