What is the Achilles Tendon?
The Achilles tendon is the largest and strongest tendon in the human body. It connects the calf muscles (gastrocnemius and soleus) to the heel (calcaneus). It helps to move the foot downwards, a movement called ‘plantar flexion’. An example of this is going up on your tiptoes. The tendon also helps to push forward when walking or running. If the tendon is torn, this is called an ‘Achilles tendon rupture’ and can occur during sport or heavy house work.
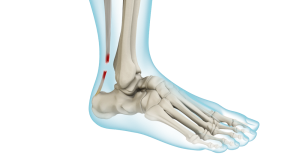
What is the cause of rupture?
Achilles tendon rupture affects about 1 in 15,000, increasing to 1 in 8,000 in competitive athletes. It can occur at any age but is most common between the ages of 30 and 50. The Achilles tendon usually ruptures without warning.
As with any muscle or tendon in the body, the Achilles tendon can be torn if there is a high force or stress placed on it. This can happen in activities which involve a forceful push off or lunging type movement, such as in football or racquet sports. The Achilles tendon can also be damaged by injuries such as falls and slips where the foot is suddenly forced into an upward pointing position (dorsiflexion).
Sometimes the Achilles tendon is already weak, making it more prone to rupture. This could be due to specific medical conditions such as diabetes; medications such as steroids and certain antibiotics such as ciprofloxacin. Ruptures can also occur when there has been long term wear and tear in the Achilles and is known as tendinopathy. Here, the tendon has degenerated and dehydrated with time and small tears form within it. This leads to weakness and therefore increased risk if rupture, even with everyday activities.
What are the symptoms?
When a rupture of the Achilles tendon occurs, you may experience a sudden pain in your heel or calf. The pain may then settle to a dull ache or it may go completely. This can be associated with a snapping or popping sound. Patients often describe the feeling as if being hit in the back of the leg, only to turn around and find no-one is there. After rupture of the Achilles tendon, there may be some swelling and bruising in your calf. It is usually difficult to walk or push off the ground properly on the injured side. You may be unable to stand on tiptoes or climb stairs.
Diagnosis
It is usually possible to detect a complete rupture of the Achilles tendon based on the history of the symptoms and clinical examination alone.
A gap may be felt in the tendon, usually a few centimetres above the heel bone. This is the normal site of the injury and is called an intra-substance tear. There may be associated swelling and bruising of the calf. The tear can also occur higher up where the calf muscles join the tendon. This is known as a musculo-tendinous tear and will often heal quicker than a tear lower down, owing to the rich blood supply from the calf muscle.
Mr Davda will examine your leg and Achilles tendon. This will require you to lie on your front on a couch,or kneel on a chair. A calf squeeze test will be performed. If the Achilles tendon is intact, the ankle will move. If there is no movement, then a rupture is very likely.
The diagnosis will be confirmed with an ultrasound scan, performed by a radiologist. The location of the rupture, size of the gap between the torn ends and if the torn ends meet when the ankle is pointing downward will be examined for.
Occasionally, the tear may be partial and usually occurs where the tendon joins the calf muscle. This injury is managed differently and usually involves resting the ankle in a boot for a few weeks.
Conservative Treatment
There are two treatment options available for Achilles tendon ruptures which are non-operative (conservative) and operative (surgical). Most patients can be successfully treated conservatively using a boot with wedges. The evidence suggests similar results to surgery without the associated complications. Occasionally, surgery may be considered, especially in cases of delayed presentation, atypical ruptures or highly active individuals.
Boot and Wedge Treatment
A boot with four wedges is typically applied to the leg. This keeps the foot pointing downwards, which keeps the two ends of the torn tendon close together, allowing them to knit together.
The demonstrates the boot with four wedges that are provided.
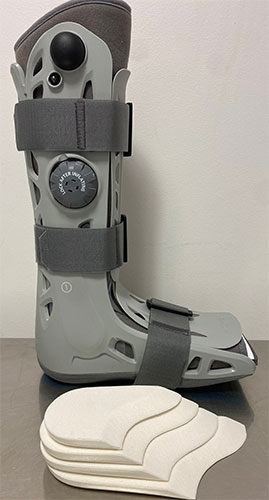
The wedges are placed under the grey foot lining that is found inside the boot as shown above

The wedges are placed under the grey foot lining that is found inside the boot as shown above

Remove the wedges every two weeks. Start with the largest and lower most wedge.

Weight bearing and walking with the boot are allowed. Crutches may be needed to help with balance. A wedge is removed every two weeks, starting with the lower most. The boot can be removed in order to have a shower, although the foot must be kept pointing down during this time. The boot must be worn at all other times, including at night. At about eight weeks, and once all the wedges have been removed, the boot should be worn for a further week. The likelihood of re-rupture remains high at this point. Thereafter the boot can be removed and normal shoes worn.
If the Achilles tear is partial, or near the calf muscle, the time in boot maybe accelerated and wedges taken out once a week. Mr Davda will advise the appropriate strategy with you in clinic.
The results of boot and wedge treatment for an Achilles rupture are extremely good for most individuals. A dedicated rehabilitation programme with a physiotherapy will begin once you have transitioned to normal footwear.
A self -administered injection will need to be taken for the duration of the boot and wedge treatment. This contains a blood thinning medication that reduces the risk of clot in the leg (deep vein thrombosis) or in the lung (pulmonary embolus). You will be shown how to do this by the pharmacy, clinic or ward staff. A guide on how to self - administer blood thinning injection is here.
Can I drive with a boot on?
Driving a manual car will not be possible whilst wearing a boot. Driving an automatic car with the right leg in a boot is not allowed. If the left leg is affected, driving may be permissible, however you are advised to check with your insurance company to ensure you are covered.
Surgical Treatment
The mainstay of treatment is the conservative route discussed above. Surgery for a torn Achilles tendon may be indicated depending on the size and gap of the tear, your activity levels and overall function. The time in cast, as well as boot/wedges remains the same as ‘conservative’ treatment highlighted above.
Before surgery
Your fitness for surgery and your ankle symptoms will be reassessed in our pre assessment clinic, which takes place prior to the date of operation. Blood tests, as well as further investigations of the heart and lungs may be required to ensure you are fit to have a general anaesthetic. If you live alone, the clinic will liaise with your GP and social services to ensure that care is in place to look after you following surgery. Occasionally, you may need to spend a few extra days in hospital whilst the services are being organised.
I kindly ask that you contact us if you suffer an insect bite, cut or bruise to the symptomatic leg in the period leading up to your surgery. Any injury to the skin in the area of your intended surgery can increase the risk of infection. You may need reassessment and surgery reorganised for another time.
On the day of surgery
You will be seen prior to surgery by Mr Davda or a member of the team to check your consent and mark the leg. Ankle tendon surgery usually takes an hour and is commonly performed under general anaesthetic. Local anaesthetic is also applied at the time of surgery to provide pain relief and numb the foot. This can last for up to a day after. The anaesthetist will discuss this further with you on the day of surgery.
Depending on the time of surgery and your recovery, you may be discharged the same day or stay in for one night, or until your post operative pain is under control and the physiotherapists are satisfied with your mobility.
The Operation – Primary Achilles Tendon Repair
Achilles tendon repair is performed with the patient lying on their front. An incision measuring several centimetres is made beside the tendon. The torn ends are brought together and repaired using a strong thick stitch. The skin is repaired using a non dissolving stitch and a cast is then applied. The foot will be placed in a position pointing downward. This position relieves tension on the repair and surrounding skin.
After The Operation
The ankle will feel numb from the local anaesthetic for the first few hours following surgery. We encourage you to take painkillers as soon as possible, as the numbness will gradually fade over time.
For the first two weeks following surgery you are advised to elevate the leg on 2-3 pillows, above the level of the chest. This will help reduce the swelling in the ankle and promote healing of the wounds. Weight should NOT be placed through the cast at this point. You will be seen in clinic about 2 weeks following surgery to check on the wound. If all is well, a boot with wedges will be applied. You will then follow the Boot and Wedge treatment regime described earlier. You will be shown how to inflate the boot and remove the wedges.
Surgery for delayed presentation or large Achilles Tendon ruptures
When an Achilles tendon rupture has occurred, and a diagnosis not made until several weeks or months later, a different surgical strategy to reconstruct the tendon may be required. The tendon to the big toe runs next to the Achilles tendon. The muscle to this tendon, known as the ‘flexor hallucis longus’, is strong and provides the next best option to replace the power lost from the calf muscles. The tendon is harvested from the back of the ankle and inserted into the heel bone. The torn ends of Achilles tendon may be too far apart to allow a direct end to end repair, hence the tendons may need to be refashioned and folded over the top of the big toe tendon to help in the repair process. Mr Davda will discuss this in greater detail with you.
In borrowing the big toe tendon, some movement to the big toe will still remain due to attachments of other tendons. It may however be weaker than before.
The time in cast and boot thereafter will be the same as for primary Achilles repair described earlier. The section on Achilles tendon rehabilitation goes through this in greater detail.
Complications of Surgery
Achilles tendon repair is a successful procedure, but there are uncommon side effects and complications to be aware of:
Swelling
This is a side effect more than a complication. Circulation around the Achilles changes after the injury and following surgery. It can take a year to improve following the operation. Regular massage of the calf muscle will alleviate this once the boot is removed.
Wound healing and infection (risk less than 1 in 100).
The wound is checked two weeks following surgery to ensure this does not occur. A course of antibiotics maybe required. The risk is increased in those who are diabetic, take medication that dampens the immune system, or smokers.
Deep vein thrombosis ( less than 1 in 100) or pulmonary embolus (less than 1/500).
Blood thinning medication will be prescribed to you for the time in cast or boot to reduce this risk. A guide on how to self administer blood thinning medication is here.
Nerve damage.
This is typically transient and may result in a change of sensation across the outer border of the foot.
Weakness.
The ankle may feel quick once the boot comes off. With good adherence to physiotherapy and exercises, the Achilles will strengthen and can take 12 months before it feels as strong as the other leg.
Re-rupture.
This risk is between 5-10% historically. More recent literature suggests about 3% and is similar to conservative management.
Common Questions
Will I able to walk after the operation?
It is best to remain NON weight bearing for the first two weeks following surgery. You will be seen in the post operative clinic at about 14 days following surgery for a wound check and removal of stitches. A boot and wedges will then be applied, and walking can begin.
When can I drive?
Patients having had the left Achilles tendon operated on, will not be able to drive. Those who have had an operation on the right side will be able to drive two weeks following surgery. Approval from your insurance company should be sought to ensure you are covered to drive.
When can I fly?
You are advised not to fly after surgery for six weeks (short haul) and 12 weeks (long haul).
When can I go back to work?
This will depend on the type of work you do. For example, if you have a desk job you may be able to return to work after two week provided you are able to rest and elevate your foot whilst sitting. If you do a physically demanding job, you will a minimum of 12 weeks off.
Can I play sport?
This is answered in greater detail in the section Achilles Tendon Rehabilitation
Physiotherapy will begin once the boot and wedges are removed, approximately 8-10 weeks following injury or surgery. Gym activity will begin thereafter, with running outdoors permissible by about week 16. Return to team and racquet sports can begin 6 months following injury or surgery, following a dedicated period pre- conditioning with a physiotherapist or gym work.
